Why Vaccines Matter: A Vital Legacy We Must Not Forget
In writing my novel The Fevered World, I spent years immersed in the history of infectious disease and vaccine development. One of my protagonists, Dr. Lorne Miller, is a physician on the front lines of the 1918 influenza pandemic. Faced with rapid, unexplained deaths around him, he resolves to stop the spiraling spread by developing a vaccine. His efforts unfold in the early, uncertain days of virology—when viruses couldn’t yet be seen, isolated, or studied, and influenza was mistakenly believed to be caused by a bacterium. Though Lorne advances the science, it will take another 27 years, until 1945, for an effective flu vaccine to be developed.
With that history in mind, I watched in 2020 as modern scientists developed the COVID-19 vaccine at unprecedented speed, using groundbreaking technologies like mRNA platforms. It was a triumph of science, but also a sobering lesson. Our pandemic exposed just how fragile public trust in science can be. Misinformation spread faster than the virus, and many refused vaccination, prolonging the crisis and leading to countless preventable deaths. As in 1918, even in the face of a deadly threat, fear and doubt undermined public health.
Today, I see further echoes of that fear in the recent measles outbreaks in Texas, New Mexico, and Kansas, and it feels like an opportunity to remember it wasn’t long ago that diseases like measles, influenza, diphtheria, and polio claimed the lives of hundreds of thousands each year. Vaccines remain one of our most powerful tools for preventing suffering and deaths, and it is crucial we remember the past and continue to value vaccines today.
Diseases That Once Devastated

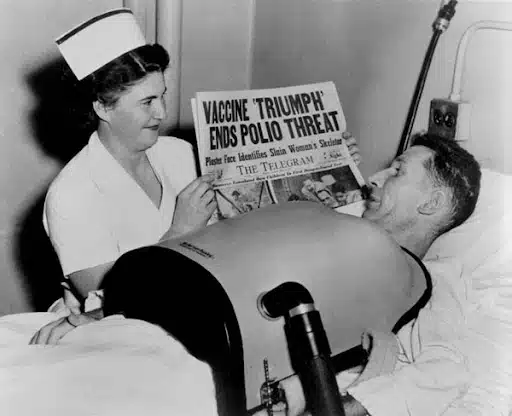
In the early and mid-1900s, like my characters in The Fevered World, families lived with the constant threat of infectious disease. Diphtheria, now virtually unknown in the U.S., killed tens of thousands of people annually until the vaccine became available in 1923. It caused suffocation, heart damage, and death, particularly in children. Measles was far from harmless. Before the vaccine in 1963, measles infected over 500,000 people annually in the U.S. Thousands died each year—including author Roald Dahl’s oldest daughter Olivia—and many more were hospitalized or left with permanent complications like brain damage or hearing loss. One of the last polio outbreaks in the United States was in 1952 and infected nearly 60,000 people, killing over 3,000 and leaving thousands permanently paralyzed, mostly children. Iron lungs filled hospitals, and communities closed swimming pools in panic. And, of course, influenza outbreaks, including the devastating 1918 pandemic I’ve written about, caused mass illness and death. In less severe years, flu still leads to tens of thousands of deaths across the U.S.
These are not ancient diseases—they were common in my childhood, feared in my parents’ childhoods— but now are being forgotten and vaccine effectiveness dismissed. Measles, for instance, was officially eliminated in the U.S. in 2000, but its return highlights how declining vaccination rates erode protection. A recent Stanford study modeled that, if current trends persist, measles could become, again, ever-present in the U.S., resulting in hundreds of thousands of cases and thousands of deaths in the coming decades
Polio Paul

When Paul Alexander was just six years old, in 1952, a virus changed his life forever. Polio left him completely paralyzed, unable to breathe on his own. For the next 72 years, he lived inside an iron lung—a metal machine that kept him alive by breathing for him, day and night. While Paul did go on to become a lawyer, a writer, and a beloved figure online—he lived with unimaginable hardship every single day. When Paul died in 2024, he was one of the last living reminders of what polio could do before there was a vaccine. Today, most of us have never seen polio or iron lungs, thanks to the vaccine.
The Risk of Forgetting Why Vaccines Matter
Ironically, the success of vaccines has made it easy to forget their importance. As diseases fade from public view, some people begin to question whether vaccines are still necessary. Fueled by misinformation and a false sense of security, vaccine skepticism has grown in recent years.
The consequences are real. In 2025, the U.S. recorded 1,288 confirmed measles cases, the highest total since 1992 and far surpassing the 285 cases reported in 2024, due largely to low vaccination rates in certain communities. These outbreaks serve as warnings: when vaccination rates drop, diseases return.
One of the most harmful myths—that vaccines cause autism—originated from a now-debunked and retracted study. Though thoroughly disproven, the claim continues to circulate online. Combating this misinformation is essential to maintaining public trust in vaccines.
The Way Forward
To protect the progress we’ve made, vaccines must remain a public health priority, supported by education, access, and strong community outreach.
We also must preserve historical memory. The stories of those who lived through polio outbreaks or lost loved ones to measles or influenza are crucial. They remind us why vaccines matter—and what’s at stake if we forget.
Come along for the ride.
Join readers who receive my occasional e-postcards, delivered to your inbox with research and history that shaped the novel, event updates, and a peek into what I’m writing next.

By subscribing, you agree to receive emails from Dee Andrews. Unsubscribe anytime. See my Privacy Policy for details.